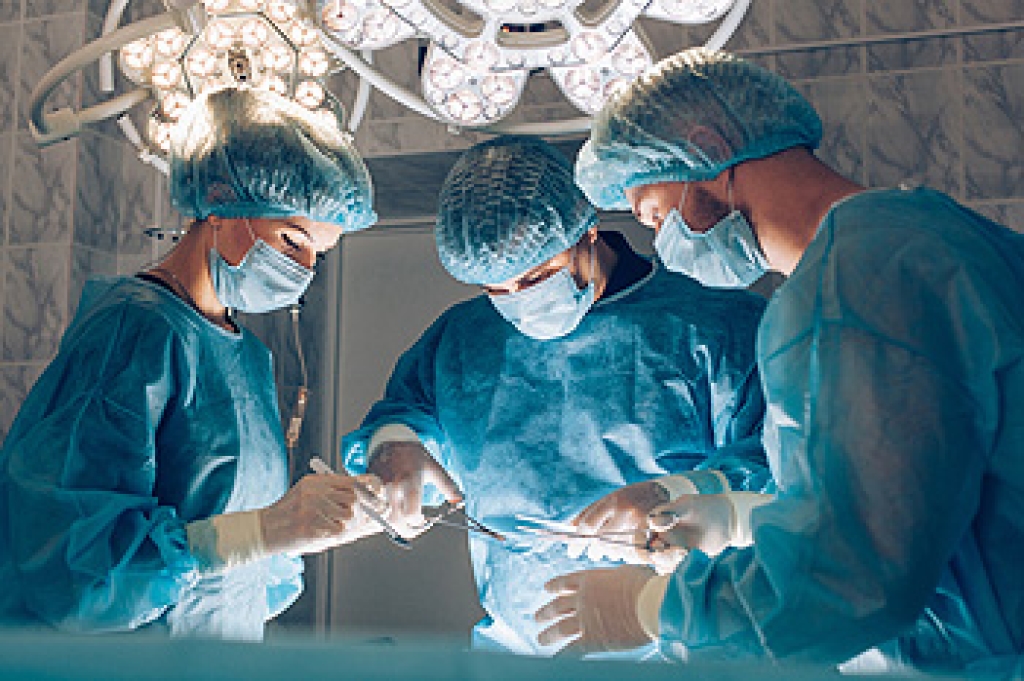
 A bunion is a bony bump on the big toe joint which may be painful, red, swollen, stiff, or sore. Over time, the bunion pushes the big toe out of alignment and towards the smaller toes. When conservative treatments, such as footwear modifications or padding the bunion do not yield results, surgery may be recommended. There are several different types of surgery for bunions. In an osteotomy, the surgeon makes small cuts in the bones to realign them. In an exostectomy, the surgeon removes the bony protrusion from the joint, but does not realign the bones. In an arthroplasty, the surgeon removes the damaged portion of the big toe joint. In an arthrodesis, the surgeon removes the arthritic surface of the joint and then uses screws of plates to close the space. Arthroplasty and arthrodesis are usually reserved for elderly patients, those who have had previous failed surgeries, and those with severe arthritis. If you have bunions, it is suggested that you consult with a podiatrist who can determine the right treatment for you.
A bunion is a bony bump on the big toe joint which may be painful, red, swollen, stiff, or sore. Over time, the bunion pushes the big toe out of alignment and towards the smaller toes. When conservative treatments, such as footwear modifications or padding the bunion do not yield results, surgery may be recommended. There are several different types of surgery for bunions. In an osteotomy, the surgeon makes small cuts in the bones to realign them. In an exostectomy, the surgeon removes the bony protrusion from the joint, but does not realign the bones. In an arthroplasty, the surgeon removes the damaged portion of the big toe joint. In an arthrodesis, the surgeon removes the arthritic surface of the joint and then uses screws of plates to close the space. Arthroplasty and arthrodesis are usually reserved for elderly patients, those who have had previous failed surgeries, and those with severe arthritis. If you have bunions, it is suggested that you consult with a podiatrist who can determine the right treatment for you.
If you are suffering from bunions, contact Dr. Edwin S. Hart of Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
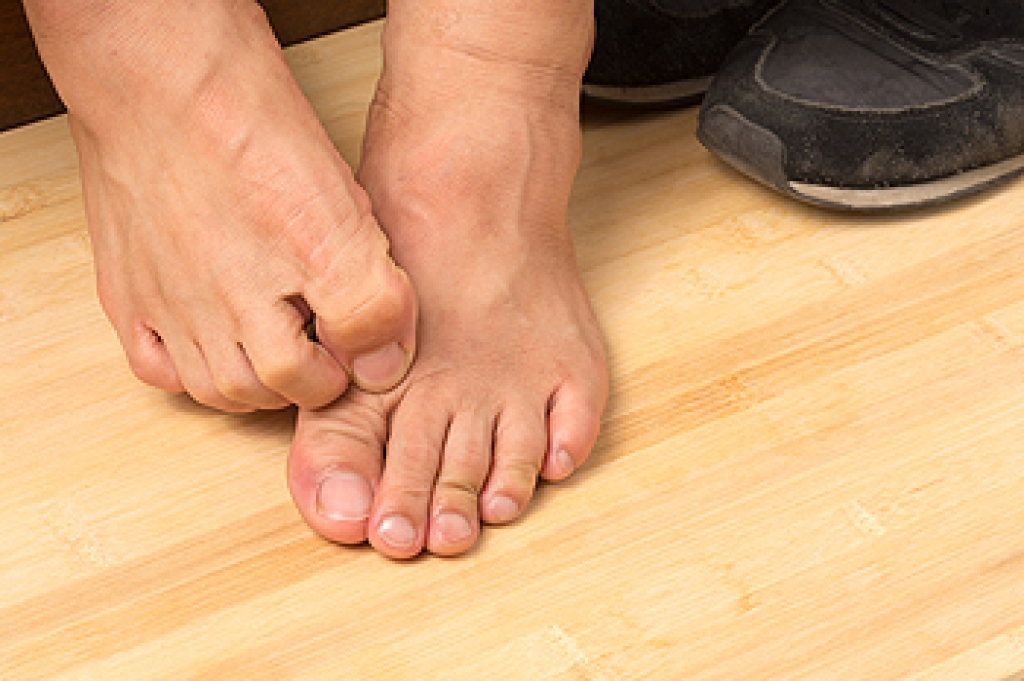
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Podiatrists often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your provider.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our office located in Bethlehem, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.





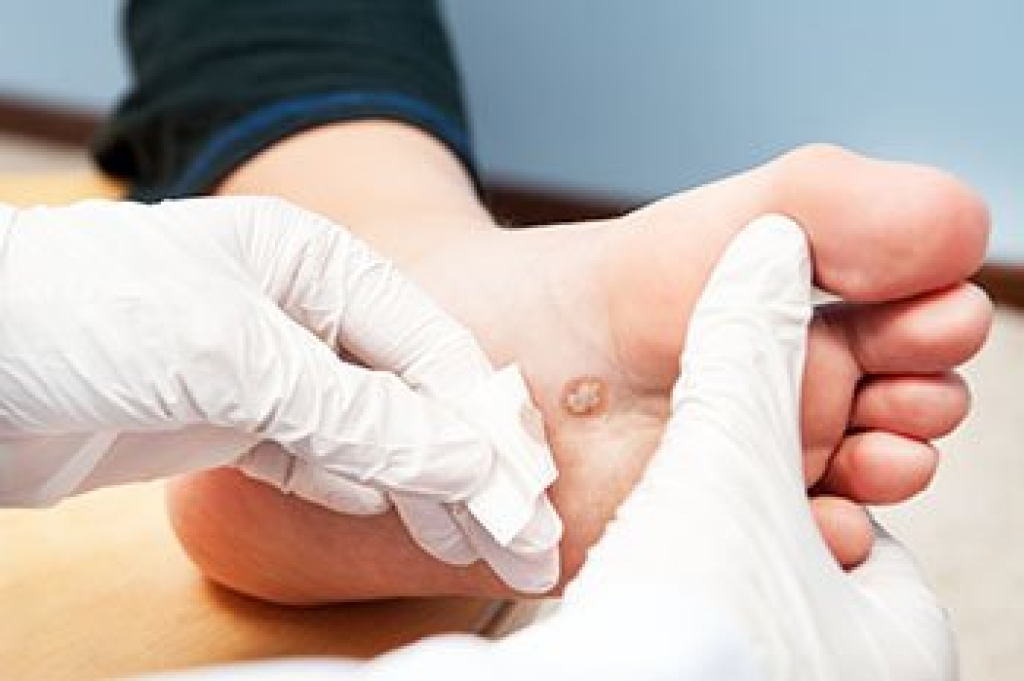

 Athlete's foot
Athlete's foot